Post written by Galen Leung, MD, from the Department of Medicine, University of Pennsylvania, Philadelphia, Pennsylvania, USA.

For this study, we wanted to evaluate the technical feasibility of salvage endoscopic submucosal dissection (ESD) after chemoradiation for locally advanced rectal adenocarcinoma in terms of rates of complete resection of residual tumor and safety profile.
Emerging evidence shows that patients with locally advanced rectal cancer have favorable outcomes in terms of clinical response and potentially complete pathological response to chemoradiation, thus potentially avoiding surgical proctectomy.
Salvage ESD can potentially be a diagnostic tool in terms of evaluating for complete pathological response to chemoradiation as well as a therapeutic option for removing the residual tumor, allowing for rectal preservation.
However, given the various technical challenges from fibrotic lesions after radiation, it was important to evaluate if salvage ESD is technically feasible and safe for removing the residual tumor.
Our study showed that when compared with standard ESD for rectal tumors without prior chemoradiation, the rate of complete tumor resection was similarly high and the adverse event rate was similarly low, supporting the technical feasibility of salvage ESD after chemoradiation for locally advanced rectal cancer.
Despite the significant number of scarred lesions in patients undergoing salvage ESD, the use of various ESD techniques (such as the pocket-creation method), electrocoagulation setting changes, traction devices, and tapered distal endoscope caps assisted in overcoming the technical challenges. Other studies have discussed the high technical feasibility and low adverse event rates of salvage ESD for esophageal squamous cell carcinoma despite increased technical challenges of mucosal and submucosal scarring and increased risk of bleeding. This had not been reported for locally advanced rectal cancer.
Interestingly, for patients who had clinical response to chemoradiation and were selected to undergo salvage ESD, upon histopathological analysis of the specimens resected by salvage ESD, 75% were no longer adenocarcinomas, indicating complete pathological response to chemoradiation. This suggests that salvage ESD may be an important tool for assessing for complete pathological response, allowing some patients to avoid surgical proctectomy.
We proposed a potential algorithm for patients who demonstrated clinical response to chemoradiation, such as no imaging or endoscopic signs of invasive disease. They may be carefully selected after multidisciplinary discussion to undergo salvage ESD for evaluation of complete pathological response. For those who demonstrate complete pathological response, salvage ESD also may be therapeutic in terms of removing the residual adenoma, enabling rectal preservation.
To assess the clinical significance of our proposed algorithm, our next study is to compare the clinical outcomes in terms of disease recurrence rates and disease-related mortality between those who underwent salvage ESD and those who proceeded with surgical proctectomy for locally advanced rectal adenocarcinoma after chemoradiation.
Currently, ESD is indicated for certain mucosal tumors and invasive cancers, including superficial submucosal invasion. However, given the significant improvement of chemoradiation in locally advanced rectal cancer and the technical feasibility of salvage ESD, the role of ESD may be potentially expanded to evaluation and therapy for locally advanced rectal cancer.
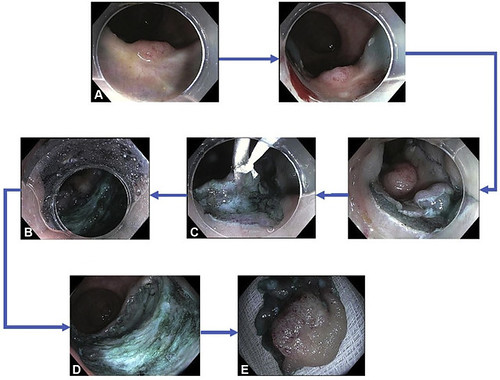 Salvage endoscopic submucosal dissection (ESD) technique. A, Post-chemoradiation residual lesion. B, The pocket-creation method of ESD. C, Traction device. D, Post-ESD defect. E, En-bloc resection specimen.
Salvage endoscopic submucosal dissection (ESD) technique. A, Post-chemoradiation residual lesion. B, The pocket-creation method of ESD. C, Traction device. D, Post-ESD defect. E, En-bloc resection specimen.
Read the full article online.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
