Post written by Radhika Chavan, MD, DNB, from the Ansh Clinic, Ahmedabad, Gujarat, India.

In this video case series, we report adverse events related to the prolonged retention of magnets and endoscopic management in children.
Three children each ingested 2 magnets of different shapes and sizes with variable periods of ingestion. They presented with abdominal symptoms, and all the cases were managed endoscopically. In 2 patients, both magnets were successfully removed. In 1 patient, the second magnet could not be removed because it became dislodged deep in the jejunum after removal of the first magnet.
All patients had delayed presentation, and all developed magnet-related fistulas (gastroduodenal: 1 patient; duodenojejunal: 2 patients). Only the patient with the gastroduodenal fistula underwent closure with through-the-scope clips. The patients with duodenojejunal fistulas were managed conservatively because they appeared to be in a well-apposed state without signs of peritonitis. There were no major adverse events related to endoscopic removal.
Over the last decade, magnet ingestion has increased significantly in children. Some parents, guardians, and health care professionals are unaware of the hazardous effects of magnet ingestion. Prolonged retention of a magnet can lead to adverse events such as a fistula, perforation, bleeding, and death (rarely), so the urgent removal of a magnet is warranted to prevent these adverse events.
All 3 cases in this case series were reported late, and all developed fistulas. This case series highlights the importance of urgent removal (within 24 hours) of a magnet to prevent these adverse events. It also highlights the use of endoscopy to remove and manage adverse events related to a magnet.
Detailed history and careful examination should be carried out before retrieval. Endoscopic retrieval is noninvasive, safe, and feasible, and it should be attempted urgently if the magnet location is amenable for endoscopic retrieval. Overlapping magnets may appear as a single object on fluoroscopy, so both antero-posterior and lateral fluoroscopic views can be taken for better interpretation (Case 2).
In this case series, 2 cases of duodenojejunal fistulas were managed conservatively. The majority of magnet-related fistulas are usually in a well-apposed state without signs of peritonitis. The decision of conservative management may be considered depending on the site, the size of the fistula, and the patient’s overall clinical status.
In conclusion, foreign body ingestion can go missing or unnoticed in children. It requires high suspicion when evaluating children with GI symptoms. Awareness among professionals involved in child health care is essential for early recognition of cases with unclear history of foreign body ingestion. Public health campaigns can help increase awareness in society about the hazardous effects of magnet ingestion.
We hope our case series highlights the importance of this often-neglected issue and the role of endoscopy in the management of magnet ingestion.
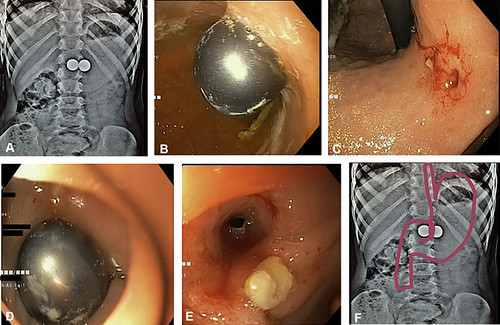
Case 1 with magnet ingestion. A, Two round, radio-opaque objects in the epigastric region on fluoroscopy. B, Endoscopy showed a magnet embedded in the stomach mucosa. C, Endoscopy showed a full-thickness defect in the gastric mucosa on the lesser curvature at the first magnet site. D, Endoscopy showed the second magnet in the duodenal bulb. E, Endoscopy showed a full-thickness defect in the duodenal mucosa in the duodenal bulb at the second magnet site. F, Schematic picturization of 2 magnets in the stomach and duodenal bulb on fluoroscopic image.
Read the full article online.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
