Post written by Rajesh Krishnamoorthi, MD, from the Digestive Diseases Institute, Virginia Mason Medical Center, Seattle, Washington, USA.

The current study is systematic review and meta-analysis to estimate the risk of progression to high-grade dysplasia and/or esophageal adenocarcinoma in patients with Barrett’s esophagus indefinite for dysplasia.
Barrett’s esophagus (BE) is a precursor lesion for esophageal adenocarcinoma (EAC). The degree of dysplasia is the most widely accepted predictor of progression in BE. An indeterminate category of dysplasia reported by pathologists is BE with indefinite for dysplasia (BE-IND). While the risk of has been well established in BE with low-grade dysplasia (LGD) and high-grade dysplasia (HGD), the natural history of BE-IND remains unclear. There is wide variation in the reported rates of malignant progression in BE-IND. As the actual risk of progression is unclear, patients with BE-IND undergo surveillance endoscopies at short intervals in clinical practice. Therefore, reliably estimating the risk of progression in BE-IND is important for both patient care and cost effectiveness.
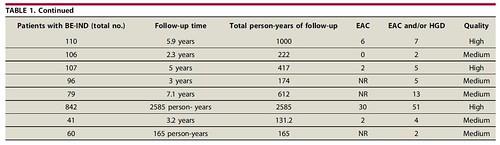
The current study is the first systematic review and meta-analysis evaluating the risk of malignant progression in BE-IND. In eight studies with 1441 patients of BE-IND, the estimated incidence of HGD and/or EAC was 1.5 per 100 person-years. The estimated incidence of EAC alone was 0.6 per 100 person-years. As our estimated progression risks in BE-IND are similar to previously reported risks in BE-LGD, surveillance intervals for BE-IND should be similar to BE-LGD.
The current study provides the best available risk estimates that may be used by gastroenterologists in counseling patients with persistent BE-IND. Patients with BE-IND should be placed on active endoscopic surveillance after their anti-reflux regimen is optimized.
Read the full article online.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
