

Post written by Young Sik Woo, MD and Kwang Hyuck Lee, MD, from the Division of Gastroenterology, Department of Medicine, Kangnam Sacred Heart Hospital, Hallym University College of Medicine, and the Division of Gastroenterology, Department of Medicine, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea.
The standard treatment of obstructive jaundice has been ERCP with biliary stenting. After failed ERCP, PTBD has been the alternative method, which is associated with a high adverse event rate and may also worsen the patient’s quality of life. EUS-guided biliary drainage has emerged as a rescue technique after failed ERCP. EUS-BD over ERCP has some advantages, including the avoidance of post-ERCP pancreatitis and tumor ingrowth problems. Therefore, EUS-BD can potentially be the first-line biliary drainage procedure, but the research results on EUS-BD are still required compared to ERCP-BD.
Only retrospective studies comparing EUS-BD with conventional ERCP as the first-line treatment option for malignant distal biliary obstruction exist, and there are some potential benefits of EUS-BD. So, a randomized trial to compare EUS-BD and ERCP-BD for primary biliary decompression in malignant biliary obstruction is needed. We did this pilot study for the future RCTs.
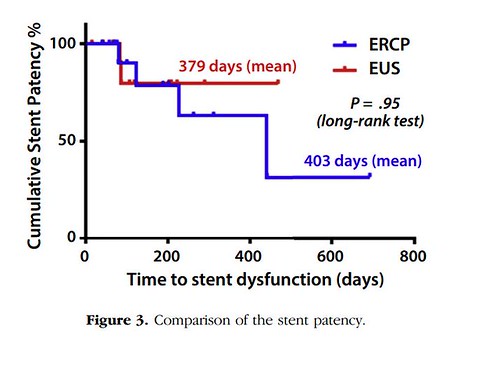
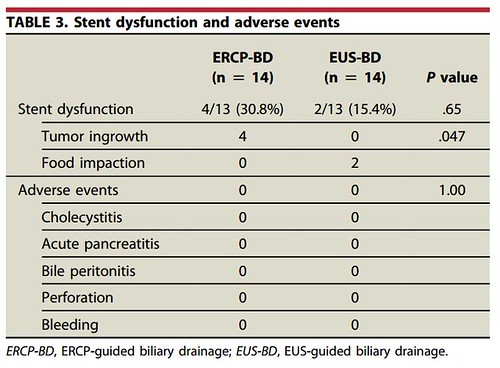
Our study is showed that there are the similar biliary drainage durability and success rates in EUS-BD and ERCP-BD. Also, no significant adverse events occurred in either group. The causes of stent dysfunction were quite different between the 2 groups. The major cause of stent dysfunction in the ERCP-BD group was tumor ingrowth and required additional stent insertion. On the other hand, the EUS-BD group had stent dysfunction because of food impaction and stent migration. The food impaction could be managed with a balloon catheter, just with pulling out the impacted food material from the inside of the stent. Interestingly, 2 patients had stent migration. No additional procedure was required because of the development of a permanent biliary-enteric fistula at the stent site.
We can confirm that the EUS-BD procedure is technically very efficient and can be safely performed, compared with ERCP-BD. EUS-BD may be a safe and promising treatment procedure for the first-line palliation of malignant biliary obstruction.
Read the full article online.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
