Post written by Tomofumi Akasaka from the Department of Gastrointestinal Oncology at Osaka Medical Center for Cancer and Cardiovascular Disease.
In this study, we used a bipolar needle-knife with a water jet function (Jet B-knife; Zeon Medical, Tokyo, Japan). After a circumferential incision, as performed for conventional ESD, esophageal lumen was filled and submucosal injection with saline solution was done by water-jet function through the Jet B-knife; soon thereafter, submucosal dissection could be performed seamlessly. Even where the identification of an appropriate dissection layer was difficult because of fibrosis, water immersion yielded a more precise procedure.
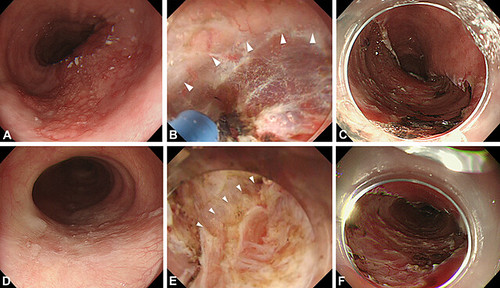
Figure 1. “Underwater” endoscopic submucosal dissection (ESD) for superficial esophageal squamous cell neoplasms. Arrowheads reveal the appropriate dissection layer, just above the muscularis propria.Wefinally achieved complete endoscopic and histologic resection without perforation.A, Flat lesion 50mm in diameter in the midesophagus. B, Submucosal dissection could be performed seamlessly soon after submucosal injection by water-jet function with a Jet B-knife. C, Ulcer bed after underwater ESD was performed without perforation. D, Flat lesion, 25 mm in diameter, adjacent to post-EMR scar in the midesophagus. E, Even where it was hard to identify an appropriate dissection plane because of fibrosis, the underwater technique helped to identify the dissection layer and yielded a more precise procedure. F, Ulcer bed after underwater ESD was performed without perforation.
Endoscopic submucosal dissection (ESD) is an effective and minimally invasive treatment for superficial esophageal neoplasms (SENs) without metastasis. However, ESD for SENs has a substantial risk of complications and difficulties. The most serious complication is perforation due to deep burn. Therefore, careful management to prevent perforation is needed. We hypothesized that use of the underwater technique might minimize thermal damage to the muscle layer and improve visualization during ESD for SENs. This study described our new strategy of “underwater” ESD for SENs and investigated its feasibility. We thought that this new method is suitable for reporting in this video section.
We believe that our strategy of underwater ESD for SENs may reduce perforation caused by deep burn, and offers an effective treatment option.
Read full text here.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
