 Post written by Ferga C. Gleeson, MD, from the Division of Gastroenterology and Hepatology, Mayo Clinic, Rochester, Minnesota.
Post written by Ferga C. Gleeson, MD, from the Division of Gastroenterology and Hepatology, Mayo Clinic, Rochester, Minnesota.
In patients with either primary or metastatic sporadic GI stromal tumors, we sought to determine the frequency of KIT and PDGFRA pathogenic alterations within paired endoscopic ultrasound cytology smears and surgical pathology specimens, Imatinib sensitivity, and the concordance of pathogenic alterations between paired specimens.
In an era of precision medicine, customized genotyping of GI stromal tumors by screening for driver mutations will become the standard of care. The National Comprehensive Cancer Network guidelines advocate the role of Imatinib as a neoadjuvant therapy in addition to its use in treating patients with metastatic or unresectable disease. The ability to stratify either primary or metastatic GISTs by mutational subtype in a preoperative or non-operative intervention setting using a targeted next-generation sequencing 2 gene mutation panel may be able to forecast Imatinib sensitivity.
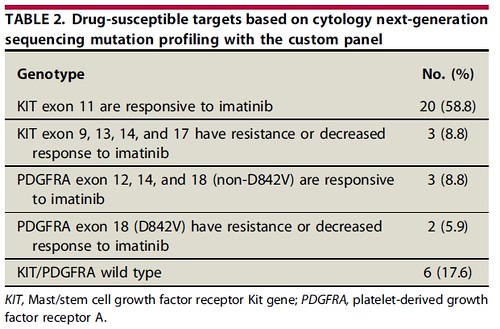
Genotyping revealed KIT and PDGFRA mutations in 68% and 15% of patients, respectively. The wild-type population did not harbor mutations in BRAF, RAS family, SDHB, SETD2, or NF1, which are found in more unusual forms of GISTs. Imatinib sensitivity based on the oncogenic kinase mutation prevalence was estimated to be 68%. Mutational concordance between paired cytology and surgical pathology specimens was 96%.
This study demonstrated the ability to use cytology smear specimens obtained via minimally invasive techniques as a suitable surrogate to surgical specimens and in turn revealed an almost absolute mutational landscape concordance between matched specimens. The combination of molecular prognostic and targeted therapy sensitivity grouping may complement conventional clinicopathologic risk stratification criteria in decision making for future GIST neoadjuvant and adjuvant therapy.
Find the article abstract here.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
