GIE Associate Editor Seiichiro Abe, MD, PhD, FASGE, FJGES, highlights this article from the April issue: “Effectiveness of self-assembling peptide in reducing bleeding after colorectal endoscopic submucosal dissection” by Takeshi Yamamura, MD, PhD, et al.

Delayed bleeding is an important adverse event after colorectal endoscopic submucosal dissection (ESD). It increases the burden of post-ESD monitoring and management.
Yamamura et al addressed this issue by evaluating whether self-assembling peptide (SAP) can reduce hematochezia and delayed bleeding after colorectal ESD.
This multicenter retrospective study included 1597 patients with 1654 colorectal ESD-related lesions at 22 institutions. After propensity score matching, 661 lesions from each group were included for comparison. The incidence of hematochezia was significantly lower in the SAP group than in the non-SAP group (16.3% vs 21.9%, P =.012). The incidence of delayed bleeding also was significantly lower in the SAP group (2.3% vs 4.5%, P = .033).
The authors further reported in multivariate analysis that SAP use was independently associated with reduced delayed bleeding (OR, 0.516; 95% CI, 0.278-0.957; P = .036). These findings support the authors’ conclusion that SAP may reduce postprocedural hematochezia and delayed bleeding after colorectal ESD.
This is a large-scale multicenter study that focuses specifically on colorectal ESD, reflecting real-world practice. In addition, the favorable association of SAP with lower hematochezia and delayed bleeding remained significant after propensity score matching, although this study has some limitations mainly because of its retrospective nature.
These findings differ from those of the PURPLE Trial,1 a randomized controlled trial that included a total of 234 hot snare colorectal and duodenal EMRs and was prematurely halted following an interim analysis. Readers should interpret the efficacy of SAP in light of the procedure (EMR/ESD and postprocedural hemostatic intervention), lesion population (organ and lesion size), and study design (hypothesis, sample size calculation, and randomized controlled trial/propensity score matching).
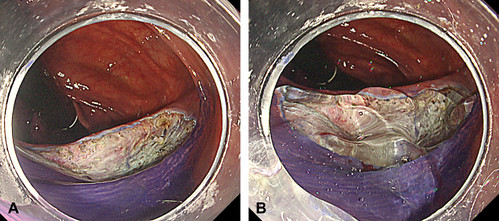
Endoscopic images after colorectal endoscopic submucosal dissection (ESD). A, A 30-mm postprocedural ulcer was observed after ESD. B, Ulcer covered with self-assembling peptide after ESD.
Read the full article online.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
- Drews J, Zachäus M, Kleemann T, et al. Multicentre randomised controlled trial of a self-assembling haemostatic gel to prevent delayed bleeding following endoscopic mucosal resection (PURPLE Trial). Gut 2025;74:1103-11. ↩︎
