Post written by Yoshihide Kanno, MD, from the Department of Gastroenterology, Sendai City Medical Center, Miyagi, Japan.
The focus of our study was to evaluate the value of routine performance of EUS-guided celiac plexus neurolysis (EUS-CPN) at an early cancer-pain stage.
EUS-CPN has been reported to be effective for patients with upper abdominal pain due to malignancy, but it has been unclear whether EUS-CPN is recommended or not, or in other words, whether EUS-CPN SHOULD be performed or not for ALL patients with pain. There have been several RCTs involving CPN without EUS-guidance but just a few with EUS-guided CPN. In most of previous studies on EUS-CPN, only single-arm outcomes or outcomes of a modified technique compared with a traditional technique have been evaluated. To debate the value of EUS-CPN itself, studies comparing outcomes with and without intervention should be referenced. However, there has been only 1 study conducted in such a way.
Patients with pancreatic cancer pain were randomly assigned to an EUS-CPN group and a medication only group. For both groups, sufficient medication was applied. The pain intensity at week 4, which was defined as the primary endpoint, was similar between the groups. Moreover, adverse effects, opioid consumption, and the survival period were similar.
The main weak point of this study is the relatively small population (24 in each group). It may have resulted in a lack of power to detect differences. However, we can say EUS-CPN does not have overwhelming power to remove pain or reduce opioid usage. EUS-CPN does not seem appropriate for ALL patients with pain in an early clinical phase. However, I do not mean that EUS-CPN is useless. It would be effective and possibly very useful for selected patients. Which patients would benefit from it and what situation is suitable for it will be confirmed in other future studies.
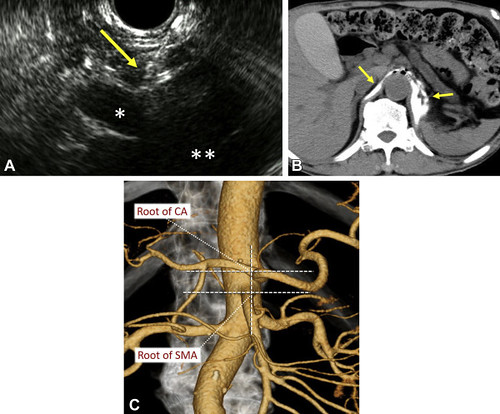
Figure 1. Procedure of EUS-guided celiac plexus neurolysis (EUS-CPN). A, EUS image of EUS-CPN. The needle (arrow) was inserted immediately above the root of the celiac artery (CA). If possible, the needle was advanced close beside the CA and deeply inserted near the superior mesenteric artery (SMA) root for injection into a broad area. *CA. **Abdominal aorta. B, CT image showing the spread of ethanol mixed with a small amount of a contrast agent (arrows). C, Six regions divided by a vertical line through the aortic center, a horizontal line through the CA root, and a horizontal line through the SMA root.
Read the full article online.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
