 Post written by Toufic Kachaamy, MD, from the Cancer Treatment Centers of America, Boca Raton, Florida, USA.
Post written by Toufic Kachaamy, MD, from the Cancer Treatment Centers of America, Boca Raton, Florida, USA.
Dysphagia palliation in non-operable esophageal cancer patients is dependent on local expertise with no clear modality favored over others. The National Comprehensive Cancer Network guidelines considers multiple modalities such as stenting, external beam radiation, brachytherapy, photodynamic therapy, cryotherapy, Argon Plasma coagulation, and YAG laser as acceptable palliation modalities. The American Society for Gastrointestinal Endoscopy recommends stenting as the preferred option; however, the stenting adverse events rate is high especially in patients who survive more than 6 months. While cryotherapy is a relatively new modality for palliation, the published data on it is very limited especially data on the safety and efficacy of cryotherapy in patients receiving systemic anti-cancer treatment. In addition, no guidelines exist on the technical details of the procedure or the timing with regards to systemic anti-cancer therapy.
We felt that this study was needed to provide acceptable technical details for using liquid nitrogen spray cryotherapy in the setting of dysphagia palliation in esophageal cancer and to determine its safety and efficacy especially in patients receiving systemic anti-cancer therapy.
This was a study of 49 patients, the majority of whom had stage 4 esophageal adenocarcinoma. They underwent a total of 120 cryotherapy sessions with a mean of 2.4 sessions per patient. 65% of patients were also receiving systemic anti-cancer therapy. The median follow-up was 5.7 months. The mean dysphagia score improved significantly from 2.6 pre-cryotherapy to 1.7 post-cryotherapy. Procedure-related adverse events occurred in 6.7%, with moderate to severe adverse events rate of less than 2%.
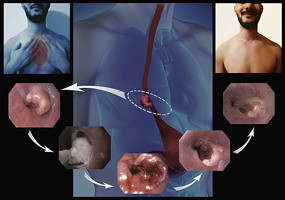
The study strength included a multi-center design with 9 operators making the results more generalizable. The main limitations of this study were the retrospective nature and the fact that quality-of-life assessment was not available on these patients. Quality-of-life assessment, in our opinion, is a more important measure of study in palliative interventions as it will better reflect the overall effect of the intervention. For example, the effect of esophageal stents on dysphagia in most studies is clearly positive while the effect on quality of life is mixed because of reflux, chest pain, and the need to sleep with the head elevated. The effect of cryotherapy on quality of life might be more favorable than the effect on dysphagia given the low incidence of adverse events typically seen with stenting.
Having the ability to offer multiple modalities for palliation is essential, especially now that cancer patients are living longer because of more effective systemic therapies. Cryotherapy is an emerging technology that seems safe and effective. Furthermore, offering cryotherapy for dysphagia palliation in patients receiving systemic therapy makes the gastroenterologist an integral part of the multidisciplinary care team. Prospective studies on the effect of cryotherapy on the quality of life of esophageal cancer are needed to better define its role and the patients who benefit the most.
Read the full article online.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
