Post written by Malay Sharma, MD, DM, from the Jaswant Rai Speciality Hospital.
This video shows the EUS features of Dieulafoy ulcer and its possible role in diagnosis of obscure overt GI bleeding. The OTSC can play an important role in the treatment of Dieulafoy ulcer.
A 50-year-old man presented with massive hematemesis. Upper-Gastrointestinal (GI) endoscopy revealed a visible vessel in the center of a small ulcer over a small submucosal bulge in the anterior wall of the first part of duodenum. EUS color Doppler showed a vessel entering the submucosa with arterial signals and confirmed the diagnosis of Dieulafoy ulcer. Endoscopic clips and adrenaline injection failed to control the bleeding. Complete hemostasis was then achieved with an over the scope clip (OTSC).
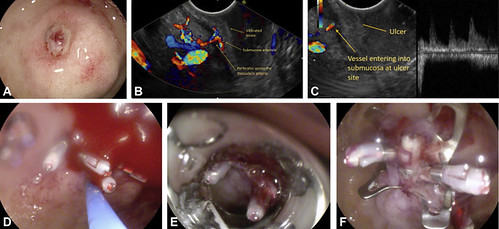
Figure 1. A, Small ulcer over a submucosal bulge in anterior wall of first part of duodenum. B, EUS color Doppler view showing submucosal vessel with feeding perforator. C, EUS pulse Doppler view showing feeding artery of submucosal arteriole. D, Hemoclips were deployed on the Dieulafoy ulcer and epinephrine was injected. E, Deploying over-the-scope clip (OTSC) over the lesion. F, OTSC over the Dieulafoy ulcer with no further bleeding. OTSC, over-the-scope clip.
Dieulafoy ulcer should be considered in differential diagnosis of small ulcer with submucosal bulge presenting with massive GI bleed. EUS has a diagnostic role in obscure upper GI bleed and can diagnose vascular anomalies which can be missed on normal endoscopy. OTSC is useful in treatment of Dieulafoy ulcer.
GI bleeding is a common condition. Rebleeding occurs in 15% to 20% of patients. This is likely related to the failure to recognize the presence of submucosal vessels at endoscopy or the failure to deliver adequate endoscopic therapy. An endoscopic approach based on the direct imaging of submucosal arterial flow and imaging-guided intervention would clearly be preferable. The specific bleeding source sometimes fails detection with routine endoscopic techniques, which suggests a potential role for EUS that allows transmural imaging. Further role of EUS should be explored as diagnostic modality for obscure upper GI bleeding.
Read the full article online.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
