Post written by Folasade P. May, MD, PhD, from the Greater Los Angeles Veterans Affairs Network and UCLA Vatche and Tamar Manoukian Division of Digestive Diseases.

African Americans see several disparities in healthcare utilization and healthcare outcomes. These disparities also occur in utilization of common gastroenterological procedures. African Americans are less likely than white Americans to undergo esophagogastroduodenoscopy (EGD) or colonoscopy when indicated for diagnostic or screening purposes, and differences in utilization may contribute to known inequities in health outcomes.
Disparities in uptake of diagnostic and screening endoscopy are multifactorial and likely include patient-level barriers to care and poor physical access to GI specialists and procedures. African Americans are also more likely to miss or be a “no show” for scheduled endoscopic procedures, as demonstrated in several recent studies.
In an effort to improve attendance for scheduled elective GI procedures in the Veterans Affairs Healthcare System (VA), our research team developed an intervention to improve overall attendance among Veteran patients recommended for endoscopy. We implemented this intervention at a single VA site and evaluated its impact on scheduling uptake and endoscopy attendance. We were also interested to see if the intervention improved uptake of endoscopy appointments specifically among African Americans.
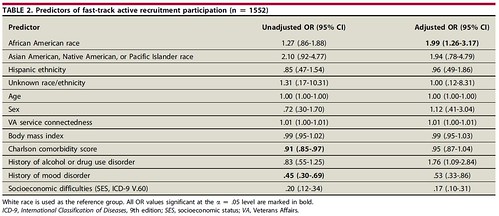
We were able to show in this study that a “fast-track” recruitment method that allows patients to take advantage of endoscopy appointments on short notice increased the overall percentage of GI clinic patients undergoing endoscopy and disproportionately improved endoscopy appointment uptake in African Americans. In fact, African Americans were twice as likely (adjusted OR, 1.99; 95% CI, 1.26-3.17) than whites to participate in the fast-track option for recommended endoscopy. Given that this population subgroup has notable under use of services, we were encouraged that the “fast-track” option was especially attractive to patients that might benefit most.
As large healthcare networks in the United States aim to reduce waste and cut costs, system efficiency is paramount. Our findings support interventions that include active recruitment as a strategy to achieve these goals and provide insight on mechanisms to improve endoscopy uptake and efficiency overall, and in African Americans in particular.
I would like to thank my research mentor, Dr. Brennan Spiegel, the Cedars-Sinai Center for Outcomes Research and Education (CS-CORE), and my co-authors.
This research was supported with a VA Health Services Research and Development Merit Award (no. IIR 12-055) for Dr. Spiegel and with a National Institutes of Health Training grant (no. T32DK07180d40) for Dr. May.
Find the article abstract here.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
