Post written by Rungsun Rerknimitr, MD, FRCP (London), FASGE, from Chulalongkorn University, Bangkok, Thailand.

Our case is about a 10-year-old girl with known tropical chronic pancreatitis with mutation at the transition c.206C>T in exon 4 of the SPINK1 gene who underwent pancreatic sphincterotomy via major papilla with pancreatic stone extraction 6 months prior.
The patient presented with a new episode of epigastric pain and elevation of serum amylase and lipase levels requiring opioid infusion to control pain. A CT scan of the upper abdomen demonstrated a new dilation of the dorsal duct only at the pancreatic head and genu suspicious for reverse pancreas divisum (Fig. 1). Dorsal duct drainage to relieve the obstruction was considered. A standard cannulation of the minor papilla failed.
A precut on the minor papilla was performed (Fig. 2), and a 0.025-inch guidewire was able to access the dorsal duct with significant difficulty to pass a 6F catheter. A dorsal pancreatogram confirmed the finding of reverse pancreas divisum with amorphous filling defect in the dorsal duct (Fig. 3).
After a 6-mm balloon pancreatic papilloplasty via the minor papilla, a single operator pancreatoscope was inserted. Pancreatoscopy revealed soft-white pancreatic protein plugs (Fig. 4) that easily gushed out to the duodenum after water irrigation.
After the procedure, the patient reported subsided pain and was able to resume a regular diet in a few days.
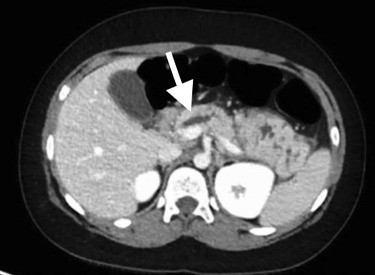
Dilated dorsal duct at the pancreatic head on a CT scan (white arrow).
Read the full article online.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
