Post written by Faisal S. Ali, MD, from the Center for Interventional Gastroenterology at UTHealth (iGUT), University of Texas Health Science Center at Houston, Houston, Texas, USA.

Our study aimed to provide further guidance on evaluating intermediate probability choledocholithiasis (IPC) in patients with cholelithiasis.
The updated American Society for Gastrointestinal Endoscopy (ASGE) guideline recommends endoscopic ultrasound (EUS), magnetic resonance cholangiopancreatography (MRCP), and intraoperative cholangiogram (IOC) as the diagnostic modalities for IPC. With increasing availability of all 3 modalities in most major institutions, we saw the need for guidance in selecting the most appropriate test for further evaluation of IPC. To this end, we designed a decision tree and conducted a cost-effectiveness analysis to identify the optimal diagnostic strategy.
Our analysis showed that performing IOC to confirm IPC in patients with cholelithiasis was the most cost-effective strategy to diagnose IPC in this patient subgroup. We measured effectiveness by (1) assigning utility scores to health states, (2) the average proportion of true positive diagnosis of IPC, and (3) the mean length of stay per strategy.
IOC was dominant in all 3 effectiveness strategies. These findings may be of value at an institutional or health system level, particularly for systems that value cost of health care and would like to devise strategies that can reduce cost. Future analyses should further assess the robustness of designating IOC as the optimal diagnostic strategy to inform society guidelines and guide clinicians at-large.
Because our analyses relied on published data for our decision model, cost(s), and effectiveness variables, the accuracy of our findings is limited by the accuracy of the current body of evidence that is used when such an analysis is carried out.
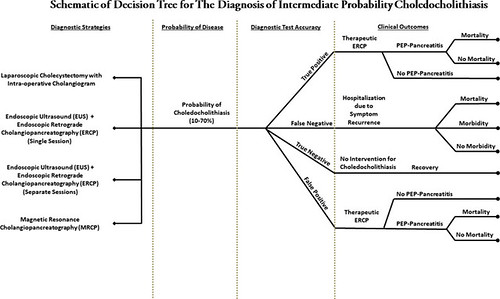
Schematic of decision tree for the diagnosis of intermediate probability choledocholithiasis. PEP, Post-ERCP pancreatitis.
Read the full article online.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
