Post written by Vivek Kumbhari, MD, PhD, from the Division of Gastroenterology and Hepatology, Department of Medicine, The Johns Hopkins Medical Institutions, Baltimore, Maryland, USA.

The goal of this study was to assess the potential value of endoscopic sleeve gastroplasty (ESG) as a treatment for obesity; this study aimed to compare weight loss outcomes of ESG with those of high-intensity diet and lifestyle therapy (HIDLT). We hypothesized that patients who underwent ESG would achieve greater %TBWL through 12 months of follow-up compared with patients enrolled in HIDLT.
As ESG continues to gain traction world-wide, a comprehensive understanding of its outcomes and its position among other non-surgical weight loss therapies is essential. The U.S. Preventative Service Task Force recommends that clinicians offer adults with a BMI >30 kg/m2 intensive, multifaceted behavioral interventions. Remarkably, however, there were no published data comparing ESG to the first-line treatment of obesity: intensive lifestyle modification therapy.
In this case-matched study, high-intensity diet and lifestyle therapy (HIDLT) patients were matched by age, sex, and BMI to ESG patients who underwent low-intensity diet and lifestyle therapy (LIDLT) following their procedure. HIDLT patients were seen biweekly for some months before transitioning to monthly visits. Weight outcomes were evaluated to a maximum of 12 months from commencement of the intervention. The results revealed that the mean total body weight loss (TBWL) in those who had undergone ESG was statistically significantly higher at 12 months compared to those who had undergone HIDLT (20.6% vs 14.3%, P<0.001). This was despite weight loss in the HIDLT cohort being extraordinarily high, with the literature generally reporting TBWL at 12 months of approximately 8%. Forty ESG patients with BMI <40 kg/m2 demonstrated statistically significantly greater TBWL at all follow-up time points. Conversely, subgroup analysis revealed no statistically significant difference in mean TBWL at 12 months in patients with BMI >40 kg/m2. Therefore, ESG is a superior weight loss approach for patients with BMI <40 kg/m2 and may be a valuable alternative for patients with BMI >40 kg/m2 who have difficulty adhering to HIDLT.
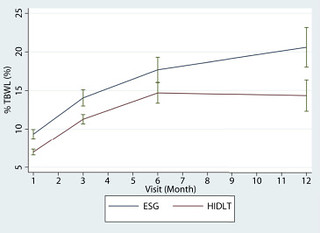
Figure 2. %TBWL at 4 time points from 1 to 12 months postprocedure in the ESG cohort and after initiation of therapy in the HIDLT cohort. ESG, Endoscopic sleeve gastroplasty; HIDLT, high-intensity diet and lifestyle therapy; %TBWL, percent total body weight loss.
Read the full article online.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
