Post written by Christoph Frank Dietrich, MD, PhD, from the Medical Department at Caritas Krankenhaus, Bad Mergentheim, Germany
With the ever growing number of cross sectional imaging, the incidental detection of small solid pancreatic tumors also increases. Until now, the general rule for the management of such pancreatic tumors has been radical surgery if considered resectable and if the patient’s fitness and comorbidities did not present contraindications. Current guidelines and international consensus recommend radical surgery for all solid pancreatic tumors as presence of pancreatic ductal adenocarcinoma is assumed. Attempting histologic or cytologic verification before surgery is not advised.
However, from our experience, we had noted that many small solid pancreatic tumors turned out not to be adenocarcinoma. Therefore, we set up a multicenter study to determine the etiology of small solid pancreatic lesions (SPL) (≤ 15 mm) to optimize the clinical management. Without preoperative diagnosis, an unacceptably large proportion of these patients would be exposed to radical surgery with significant mortality and morbidity.
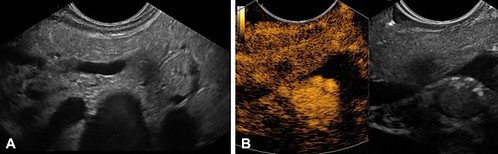
In our study, the majority of small solid pancreatic tumors of less than 15 mm (63%) were not pancreatic ductal adenocarcinoma and, therefore, in most cases would not require radical pancreatic surgery. In our cohort of 394 small solid pancreatic tumors (
Future prospective studies should focus on the characterization of small solid pancreatic tumors using modern advanced ultrasound imaging techniques and EUS-guided sampling techniques to avoid unnecessary radical surgery in patients without adenocarcinoma. While large solid pancreatic tumors are more likely to be considered for direct surgery, the finding of small solid pancreatic tumors should prompt further investigation before surgery to determine the etiology of the lesion. Contrast enhanced endoscopic ultrasound seems the most suitable imaging modality to guide further management. Especially in patients with iso- or hypervascularized SPL ≤ 15 mm, tissue diagnosis should be attempted by performing EUS-guided sampling.
Find the article abstract here.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
