 Post written by Tae Jun Song, MD, PhD and Sang Soo Lee, MD, PhD from the Department of Internal Medicine, University of Ulsan College of Medicine, Asan Medical Center, Seoul, South Korea
Post written by Tae Jun Song, MD, PhD and Sang Soo Lee, MD, PhD from the Department of Internal Medicine, University of Ulsan College of Medicine, Asan Medical Center, Seoul, South Korea
Preoperative biliary drainage (PBD) with stent placement has been commonly used for patients with malignant biliary obstruction. In PBD, the placement of fully-covered self-expandable metal stents (FCSEMSs) may provide better patency duration and a lower incidence of cholangitis compared with plastic stents. So, we compared the outcomes of PBD with either plastic stents or FCSEMSs in patients with distal malignant biliary obstruction. FCSEMSs have been thought to be superior to plastic stents during PBD because occlusion and need for stent exchange were rare in PBD with FCSEMSs. However, to date, no randomized study has prospectively compared the outcomes of PBD with plastic stents versus FCSEMSs.
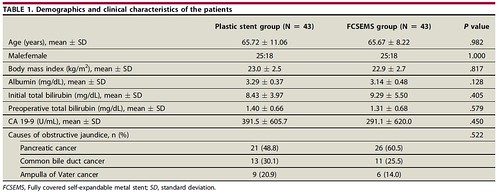
Our study was designed to determine whether PBD with FCSEMSs was associated with fewer PBD- and surgery-related adverse events compared with those for plastic stents in our routine clinical practice. We believed that the use of FCSEMSs with wider lumen might somehow considerably change the outcome of PBD, as shown in previous retrospective studies that indicated its advantages in providing rapid biliary decompression and a significant reduction in preoperative reintervention rates compared with plastic stents. However, the present study shows that the outcomes of PBD with plastic stents and FCSEMSs were not different in patients with distal malignant biliary obstruction who had planned to undergo early primary surgery. Further prospective randomized studies that compare the outcomes of plastic stents and FCSEMSs in various clinical situations such as a neoadjuvant therapy setting are necessary. Our study suggests an option for preoperative biliary drainage. The need for PBD and choice of the most adequate drainage method should be decided considering the patients’ symptoms, time to surgery, and cost-effectiveness.

Find the article abstract here.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
