
Satoki Shichijo and Yoshihiro Hirata from the Department of Gastroenterology, Graduate School of Medicine, The University of Tokyo, describe this Original Article published in GIE.
We reported a retrospective, endoscopy-based, long-term cohort study to elucidate the risk factors for gastric cancer development after Helicobacter pylori (H. pylori) eradication. We assessed histologic and endoscopic findings of gastritis and performed H. pylori eradication therapy in 748 patients without a history of gastric cancer. Among them, a total of 573 patients underwent follow-up endoscopy over 6.2 ± 4.8 years. Gastric cancer developed in 21 (20 intestinal type). Patients with histologic intestinal metaplasia or severe endoscopic atrophy were at increased risk of gastric cancer development after H. pylori eradication.
Helicobacter pylori eradication therapy is effective at reducing the incidence of gastric cancer, and eradication therapy prevails. However, gastric cancer still develops after eradication. Risk factors for gastric cancer after eradication were not fully understood.
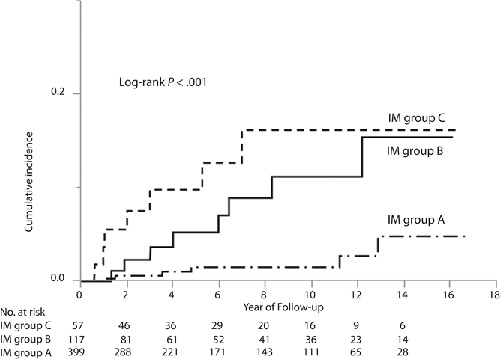
Our study showed that not only endoscopic atrophy but also histologic intestinal metaplasia are risk factors for gastric cancer development after H. pylori eradication. Of 21 patients who developed gastric cancer after eradication therapy, 20 (95%) were intestinal types, and only one was diffuse type, similar to previous reports showing a predominance of intestinal gastric cancer after eradication.
The combination of eradication therapy, which reduces gastric cancer incidence (especially of diffuse type) and intensive follow-up for high-risk patients (those with histological intestinal metaplasia and severe endoscopic atrophy) will lead to decreasing gastric cancer deaths.
Find the article abstract here.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
