 Lorenzo Fuccio, MD, from the Department of Medical and Surgical Sciences, S.Orsola-Malpighi University Hospital, in Bologna, Italy discusses this Original Article, “Development of a prediction model of adverse events after stent placement for esophageal cancer.”
Lorenzo Fuccio, MD, from the Department of Medical and Surgical Sciences, S.Orsola-Malpighi University Hospital, in Bologna, Italy discusses this Original Article, “Development of a prediction model of adverse events after stent placement for esophageal cancer.”
We conducted a retrospective analysis of a large database including 267 patients with dysphagia owing to esophageal cancer and treated with covered and partially covered metallic stent. The main aim of our study was to identify factors influencing the risk of long-term adverse events and build a predictive model to use in the daily practice.
This study represents the first attempt to develop a predictive model of risk of adverse events in patients with dysphagia due to esophageal cancer and treated with stent placement. 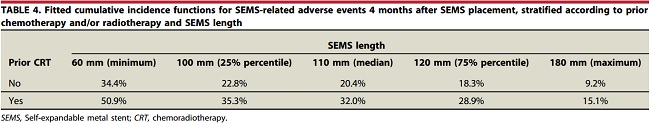
The multivariable analysis identified 2 factors significantly influencing the risk of adverse events. Prior chemo-radiotherapy (CRT) significantly increased the risk with a reported hazard ratio (HR) of 1.687 (95% CI: 1.076-2.644). Of note, all 10 cases of esophageal fistula developed in patients with a prior history of CRT. Conversely, the stent length resulted as a protective factor (HR 0.884; 95% CI, 0.798-0.980 for every 10-mm length increase). This latter finding was never been reported.
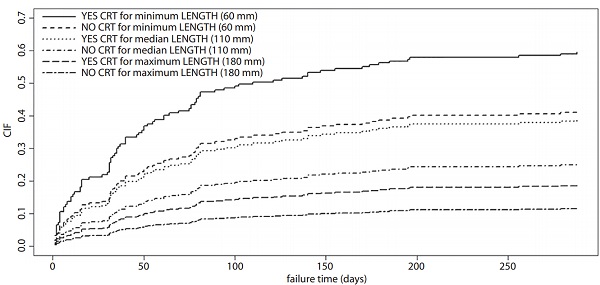 Figure 1. The estimated cumulative incidence functions for the event adverse event rate for participants who did not receive any therapy and for those who received prior chemotherapy and/or radiotherapy, stratified according to self-expandable metal stent length (60 mm, 110 mm, and 180 mm). CIF, cumulative incidence functions; CRT, chemoradiotherapy.
Figure 1. The estimated cumulative incidence functions for the event adverse event rate for participants who did not receive any therapy and for those who received prior chemotherapy and/or radiotherapy, stratified according to self-expandable metal stent length (60 mm, 110 mm, and 180 mm). CIF, cumulative incidence functions; CRT, chemoradiotherapy.
Several hypotheses can be proposed in order to explain this unexpected association: a longer stent might be less prone to migrate because of a major stability and to be occluded by tumor overgrowth; furthermore, the radial force might be differently distributed across the stent, with lower force at both ends, reducing the risk of inflammatory response in the surrounding normal tissue. Since this is the first time that stent length is reported as a possible protective factor, this should be investigated in further studies.
Read the abstract for this article online.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
