 Maria Pellisé, MD, PhD, from the Department of Gastroenterology and Hepatology, at the University of Sydney in New South Wales, Australia shares this Original Article, “The influence of clips on scars after EMR: clip artifact.”
Maria Pellisé, MD, PhD, from the Department of Gastroenterology and Hepatology, at the University of Sydney in New South Wales, Australia shares this Original Article, “The influence of clips on scars after EMR: clip artifact.”
In this study, we aimed to describe the influence of clips on the EMR scar. Endoscopic clips are increasingly used to mitigate the risk of delayed bleeding.
In our daily practice we observed that after clipping a defect, endoscopic appearance of post-EMR scar was sometimes altered. Colonoscopic assessment of recurrent or residual neoplasia might be interfered by the presence of it. We considered it was important to describe this phenomenon in order to avoid misinterpretation during post-EMR surveillance colonoscopies. 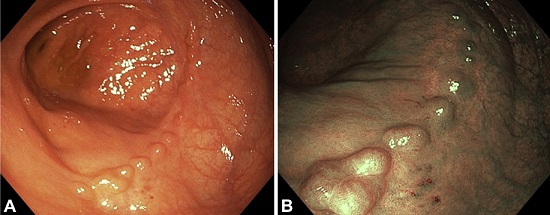
Figure 5. Multiple nodules secondary to clipping. Ten clips were used to close the defect. A, Notice the linear disposition of the nodules with white light endoscopy. B, Linear disposition of the nodules with narrow-band imaging.
Post-EMR scar clip artifact can be present in almost 50% of EMR sites that have been clipped. This can appear as a residual clip surrounded by granulation tissue or as nodules of elevated normal mucosa. It is not associated with the size of the defect, location or histology of the removed polyp. Interestingly, the presence of deep mural injury is not related to the presence of clip artifact. Conversely, prophylactic closure with clips to prevent bleeding was significantly associated with clip artifact. This is most likely because closing the whole mucosal defect could result in substantial tissue tension as the edges are drawn together, particularly if the mucosal defect is wide, in comparison with focal closure of a muscularis propia defect were the length of the width of closure is much smaller.
The recognition and differentiation of nodules related to granulation and clip artifact may avoid unnecessary additional therapy, reduce inappropriate surveillance and allay patient anxiety regarding recurrence. All colonoscopists should be aware of this phenomenon. It is important to recognize and differentiate it from recurrence in order to avoid unnecessary treatment or inappropriate surveillance recommendations. Future research, evaluating the accuracy of endoscopic imaging in discriminating it from recurrence is warranted.
Read the abstract online here.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.

Dear Prof. Pellisé,
Congratulations on your nice and original publication.
During a follow-up colonoscopy after EMR, should we bother with the presence of clips and remove then?
Thank you for your comment. The clips can hinder the scar inspection. In that sense, we would recommend to remove them to have a better view of the scar. However, you always have to consider as well the risk of complications, efficiency and or time-waste. The decision has to be taken case by case.
Dear Prof. Pellisé,
Thank you for your thoughtful comment.