 Martin C.S. Wong, MD, MPH, from the Institute of Digestive Disease and the JC School of Public Health and Primary Care at the Chinese University of Hong Kong in Shatin, Hong Kong, HKSAR, China discusses this Original Article, “Association of distal hyperplastic polyps and proximal neoplastic lesions: a prospective study of 5613 subjects.”
Martin C.S. Wong, MD, MPH, from the Institute of Digestive Disease and the JC School of Public Health and Primary Care at the Chinese University of Hong Kong in Shatin, Hong Kong, HKSAR, China discusses this Original Article, “Association of distal hyperplastic polyps and proximal neoplastic lesions: a prospective study of 5613 subjects.”
The objective of this study to evaluate if subjects detected having distal hyperplastic polyps (HPs) had significantly higher risk for proximal neoplasia when compared to those without. As flexible sigmoidoscopy (FS) is one of the recognized screening modalities for colorectal cancer, this study aims to inform physicians on subsequent follow-up when a distal lesion is detected in FS. Current evidence of whether distal HPs are markers of proximal neoplasia (PN) or Proximal Advanced Neoplasia (PAN) is mixed.
It is observed that many physicians still refer patients with distal HPs alone for colonoscopy. From existing literature, formal guidelines do not endorse distal HPs as markers of PN or PAN. Briefly, 14 out of 17 prospective colonoscopy studies do not report any association between distal HP and PN or PAN. The mixed findings are also evident — among 4 published meta-analyses, 2 concluded that there was an association between distal HP and PN; 1 demonstrated an association between distal adenomas and PN, and 1 showed no association between distal HPs and PN or PAN. Hence existing evidence does not seem adequate to support physicians’ decision when a distal HP was detected in colonoscopy – the main question is “should patients with distal HP be referred routinely for direct colonoscopy?” 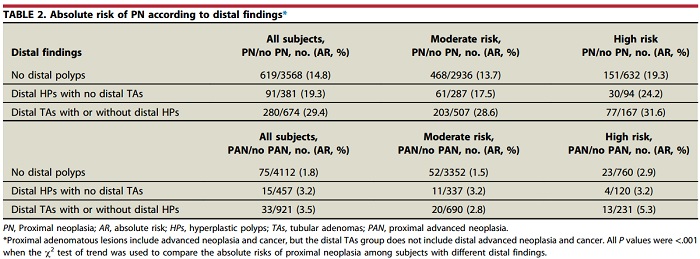
This prospective colonoscopy study including 5,613 screening participants showed that the absolute risk of PN among subjects without HP (14.8%) was not significantly lower than those with distal HPs (19.3%). From multivariate regression analysis, there is no difference in risk of PN or PAN between those with distal HP vs. those without. These results implied that routine referral of subjects with distal HPs detected (eg, by FS) might not be necessary in clinical practice. These findings are important to inform physicians on the subsequent management of distal HPs detected by screening FS.
The implication of this study is mainly on subjects who receive flexible sigmoidoscopy only without any information on the presence of lesions in the proximal colon. The findings do not apply among those who have received colonoscopy already, as there is no point to predict whether any PN/PAN exists. The “optimal” study design should be a two-step approach, where study participants are recruited to undergo FS first followed by colonoscopy. Nevertheless, such an approach may need 2 separate endoscopy visits; require much more resources, and might lead to a low response rate.
Fine the abstract online.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
