 Mikihiro Fujiya, MD, PhD and Kazuyuki Tanaka, MD from the Division of Gastroenterology and Hematology/Oncology, Department of Medicine, Asahikawa Medical University in Asahikawa, Japan present this Original Article “Efficacy and adverse events of EMR and endoscopic submucosal dissection for the treatment of colon neoplasms: a meta-analysis of studies comparing EMR and endoscopic submucosal dissection.”
Mikihiro Fujiya, MD, PhD and Kazuyuki Tanaka, MD from the Division of Gastroenterology and Hematology/Oncology, Department of Medicine, Asahikawa Medical University in Asahikawa, Japan present this Original Article “Efficacy and adverse events of EMR and endoscopic submucosal dissection for the treatment of colon neoplasms: a meta-analysis of studies comparing EMR and endoscopic submucosal dissection.”
We herein performed a meta-analysis of the literature to clarify how to select the optimal endoscopic procedure for removing colon neoplasms.
The removal of colon adenomas and early-staged cancer is considered to prevent the development of advanced cancer. Both endoscopic mucosal resection (EMR) and endoscopic submucosal dissection (ESD) are frequently used to remove colon neoplasms. EMR is a minimally invasive and easy-to-learn procedure for removing colon neoplasms. However, the risks of local recurrence after EMR were reported in cases with piecemeal excision, invasive pathology, and larger lesions. ESD is another procedure that is frequently used for removing large lesions. The curability of ESD is considered to be sufficiently high for removing colon tumors, however, the safety of ESD is inferior to that of EMR and the longer procedure time is considered to be another disadvantage of ESD.
Several comparative studies concerning the usefulness between EMR and ESD were previously reported, however, it is not yet clear how to select the optimal endoscopic procedure for individual lesions. We therefore conducted the present study in order to compare the efficacy and adverse events between EMR and ESD.
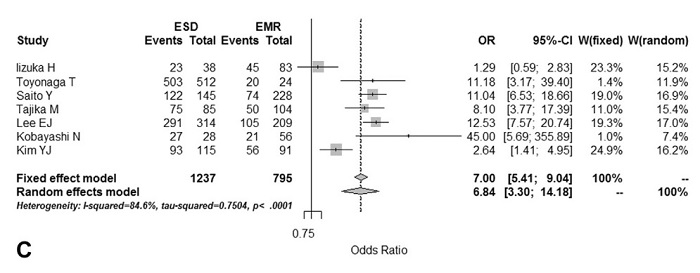
Figure 2. Forest plots were used to verify the relative strength of the diagnostic value of each procedure. The results regarding the rate of en bloc resection are shown. ESD, endoscopic submucosal dissection; SD, standard deviation; MD, mean difference; CI, confidence interval; W, weight; OR, odds ratio.
The present study indicates that the rate of en bloc resection and curable resection was significantly higher, and the rate of recurrence was significantly lower in the ESD group than in the EMR group. However, the procedure time was significantly longer and the rate of additional surgery and perforation were significantly higher in the ESD group, thus suggesting that the indications for ESD should therefore be rigorously determined in order to avoid such problems.
More RCTs with standardized procedures must be conducted in order to identify the proper use of EMR and ESD for removing colon neoplasms. We hope that our findings will help to determine the optimal procedure for removing colon neoplasms.
Read the abstract for this article online.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
