Emo E. van Halsema, MSc discusses this Original Article “Perforation in colorectal stenting: a meta-analysis and a search for risk factors” from the June issue.
We performed a meta-analysis of the literature to identify risk factors for perforation from colonic stent placement. A total of 86 studies published between 2005 and 2011 were selected, including 4086 patients who underwent a colorectal stent placement procedure. We determined the perforation rates of different variables, including stent design, stricture etiology (malignant or benign), stricture dilation and concomitant chemotherapy, including the use of bevacizumab.
Colorectal stent placement is associated with an increased risk of colonic perforation. Several risk factors for the occurrence of perforation have been suggested in the literature. However, the sample sizes and number of events are usually too small to statistically confirm these supposed risk factors. Therefore we conducted a meta-analysis of the available literature.
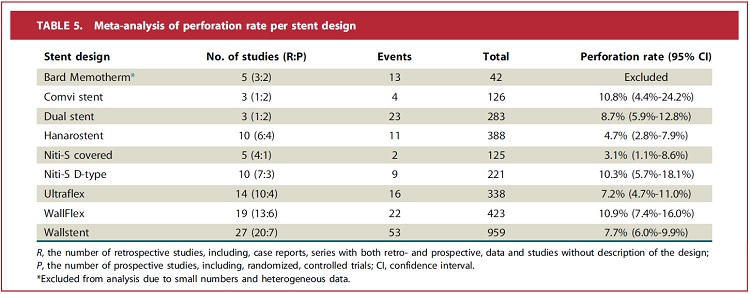
After meta-analysis, the overall risk of colonic perforation in the literature was 7.4%. Almost 70% of the perforations occurred in the first week after stent placement. Between eight different stent designs the perforation rates ranged from 3.1%-10.9%. Further statistically significant risk factors for perforation that were identified by meta-analysis were: benign strictures (18.4%), reintervention dilation during the course of stenting (20.4%) and concomitant treatment with the anti-angiogenic agent bevacizumab (12.5%). Pre-stent dilation (8.2%) and chemotherapy without bevacizumab (7.0%) were not associated with an increased perforation risk. The wide variation in perforation rates between the different stent models suggests that the stent design could be a causative factor for the occurrence of perforation. However, no firm conclusions can be drawn because these outcomes are limited by heterogeneity, possible confounders and the considerable proportion of missing data in the literature. Nevertheless, this study provides insight into perforation after colorectal stent placement. To learn more, we call for more detailed reporting on perforation in future research, including data on the circumstances in which perforation occurs, subgroup analyses to identify risk factors, pathological reports, and clinical and oncological outcomes after perforation.
Read the abstract for this article online.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
