Akira Horiuchi, MD from Showa Inan General Hospital in Komagane, Japan writes about his Original Article “Removal of small colorectal polyps in anticoagulated patients: a prospective randomized comparison of cold snare and conventional polypectomy” from the March issue.
No delayed bleeding occurred after cold snare polypectomy whereas endoscopic hemostasis for immediate and delayed bleeding was required following conventional polypectomy. The presence of injured submucosal arteries with conventional polypectomy was significantly more frequent than with cold snare and is hypothesized to be responsible for the difference in delayed bleeding. Cold snare polypectomy is preferred if small colorectal polyps are to be removed from anticoagulated patients.
For the millions of patients who use anticoagulants, or blood thinners, polypectomies carry higher risk because of bleeding that occurs during excision of the polyp and recovery. By comparing 2 kinds of polypectomies, we found that a method called a “cold snare” technique is safer for patients on anticoagulants. This study compared the bleeding associated with the conventional polypectomy technique and the cold snare technique.
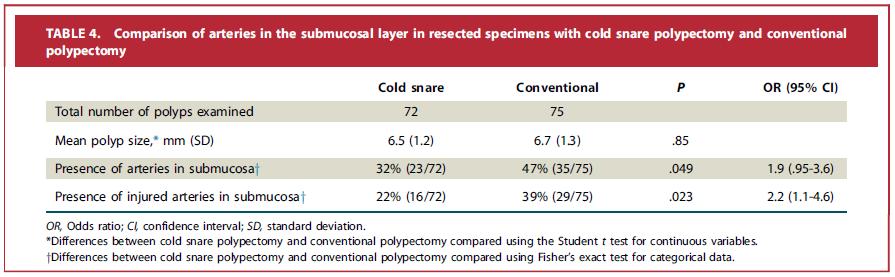
We speculated that the cause of delayed bleeding would be related to injury of blood vessels in the submucosa layer caused by electrocautery. Arteries were detected more often in the submucosal layer in the Conventional group then in the Cold group (47% vs 32%, P=.049). However, the difference was of borderline significance, possibly related to the small sample size. Importantly, injured submucosal arteries were seen significantly less frequently in the Cold group than following Conventional polypectomy (22% vs 39%, P=.023) (Table 4). This difference is consistent with the increase in delayed bleeding associated with conventional compared to cold polypectomy and with our previous study showing that conventional polypectomy was associated with more abdominal symptoms after polypectomy than following cold snare polypectomy.
Find this article on pages 417-423 of the journal or online.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
