Post written by Chawin Lopimpisuth, MD, from the Department of Medicine, University of Miami/Jackson Health System, Miami, Florida, and Sean Bhalla, MD, from the Division of Gastroenterology and Hepatology, University of Colorado Anschutz Medical Campus, Denver, Colorado, USA.

This study aimed to compare the safety of covered self-expandable metal stents (CSEMSs) versus uncovered self-expandable metal stents (USEMs) in the management of distal malignant biliary obstruction, with particular focus on the incidence of postprocedural cholecystitis.
Conflicting data exist regarding the risk of postprocedural cholecystitis after CSEMS versus USEMS placement. Although earlier studies suggested a higher risk with CSEMSs, recent meta-analyses have not demonstrated a significant difference. In addition, the 2024 “American Society for Gastrointestinal Endoscopy guideline on the role of endoscopy in the diagnosis and management of solid pancreatic masses: summary and recommendations”1 states that in distal malignant biliary obstruction, based on the literature, there is no difference between CSEMSs versus USEMSs. However, the guidance recommends placing self-expandable metal stents below the cystic duct orifice.

In prior studies, adverse events such as cholecystitis were often not the primary outcome. Key confounders, including history of cholecystectomy, were not included. Given the growing emphasis on procedure-related safety and additional studies performed, we believe a focused and refreshed meta-analysis of the adverse event was warranted.
Our findings revealed a significantly elevated risk of postprocedural cholecystitis, approximately 2-fold higher with CSEMSs than with USEMSs, which persisted after adjustment for prior cholecystectomy in our subgroup analysis. To our knowledge, this is the first meta-analysis to highlight the exclusion of patients with a history of cholecystectomy and to demonstrate a significantly higher risk of cholecystitis associated with CSEMS placement. Our study also showed a significantly lower risk of tumor ingrowth and a higher risk of stent migration in the CSEMS group than with the USEMS group. Despite prior reports, our analysis did not find a significant difference in the risk of postprocedural pancreatitis between the 2 stent types.
These data support the need for individualized stent selection in patients with malignant biliary obstruction. In patients with prior cholecystectomy, CSEMSs can be placed safely, but in those patients with indwelling gallbladder, thoughtful consideration must be made when choosing CSEMSs versus USEMSs to minimize adverse events and prevent delays in oncologic management.
Future studies that compare different types of CSEMSs would be beneficial as current available stents have differences in antimigratory properties and tensile force, which may play a role in postprocedural cholecystitis. Moreover, a study that analyzes and takes into account several factors such as location of stent placement in relation to the cystic duct, cystic duct visibility on cholangiogram/cholangioscopy prior to stent placement, presence of malignancy at the level of the cystic duct orifice, and presence of gallbladder distension could potentially help dictate stent selection and placement to prevent further adverse events.
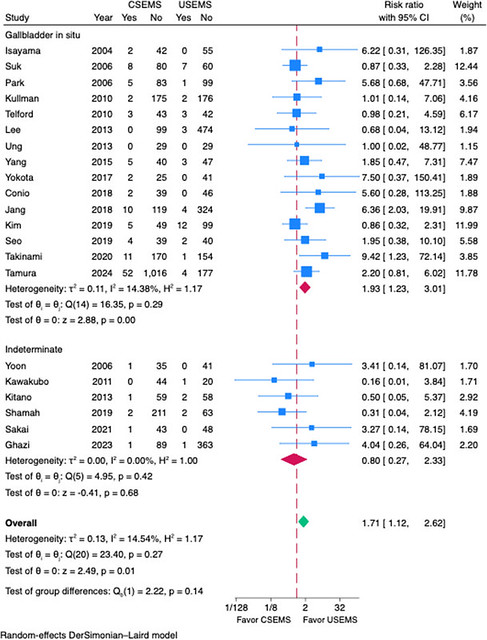
Forest plot of the risk ratio of postprocedural cholecystitis rate for presence of gallbladder in situ.
Read the full article online.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
- ASGE Standards of Practice Committee; Machicado JD, Sheth SG, Chalhoub JM, et al. American Society for Gastrointestinal Endoscopy guideline on the role of endoscopy in the diagnosis and management of solid pancreatic masses: summary and recommendations. Gastrointest Endosc 2024;100:786-96. ↩︎
