Post written by Ricardo Almeida, MD, from the Universidade Federal de São Paulo, São Paulo, Hugo Guedes, MD, Liliana Mendes, MD, and Carlos Rassi, MD, from the Department of Gastroenterology, Hospital Sírio-Libanês, Brasília, Brazil, Roberto Simons-Linares, MD, MSc, from the Department of Gastroenterology and Hepatology, Cleveland Clinic, Cleveland, Ohio, Prabhleen Chahal, MD, MASGE, FACG, and Matheus C. Franco, MD, MBA, MSc, PhD, from the Division of Gastroenterology and Nutrition, Department of Medicine, UT Health San Antonio, San Antonio, Texas, USA.

We present the case of a 62-year-old woman with a history of Roux-en-Y gastric bypass (RYGB) who developed hyperammonemic encephalopathy—a rare but life-threatening metabolic adverse event—resulting from severe weight loss, sarcopenia, and small intestinal bacterial overgrowth.
Following partial response to lactulose and rifaximin, and given the patient’s high surgical risk, she underwent EUS-guided gastrogastrostomy with placement of a 20-mm lumen-apposing metal stent (LAMS) (Hot AXIOS; Boston Scientific, Mass, USA) to restore foregut continuity. The procedure led to rapid normalization of ammonia levels (283 to 103 μmol/L), resolution of encephalopathy, and progressive weight gain. The LAMS was removed at 8 months; at 2-month follow-up, the gastrogastric fistula remained patent with sustained clinical benefit and normal ammonia levels (42 μmol/L).
Hyperammonemic encephalopathy following RYGB is a rare and under-recognized condition that can be fatal if not promptly managed. Although surgical reversal is the definitive treatment, it carries significant morbidity in malnourished or medically complex patients.
This case illustrates, to our knowledge, the feasibility and safety of EUS-guided endoscopic reversal using a LAMS as a minimally invasive alternative—potentially life-saving for patients who cannot tolerate open surgery. We hope this video highlights a technically accessible approach that expands the therapeutic toolkit available to advanced endoscopists managing complex postbariatric adverse events.
This case offers several important takeaways for advanced endoscopists: (1) postbariatric hyperammonemic encephalopathy should be recognized as a distinct clinical entity, even in the absence of underlying liver disease; (2) EUS-guided gastrogastrostomy with a LAMS is technically feasible and can produce durable results, with fistula patency maintained even after LAMS removal; (3) a structured multidisciplinary approach—including neurology, nutrition, and gastroenterology—is essential for optimal outcomes; and (4) endoscopic reversal preserves the option of future surgical revision, maintaining long-term management flexibility. Given the growing global bariatric population, familiarity with this technique is increasingly relevant for interventional endoscopists.
This case underscores the importance of advanced endoscopic expertise in managing complex postbariatric metabolic adverse events. We acknowledge the experimental nature of this approach and the need for larger prospective studies to define patient selection criteria, optimal LAMS duration, and long-term outcomes. Endoscopic reversal should currently be reserved for carefully selected patients at experienced centers. We hope this video contributes to the growing literature on minimally invasive strategies for RYGB reversal and stimulates further research in this area.
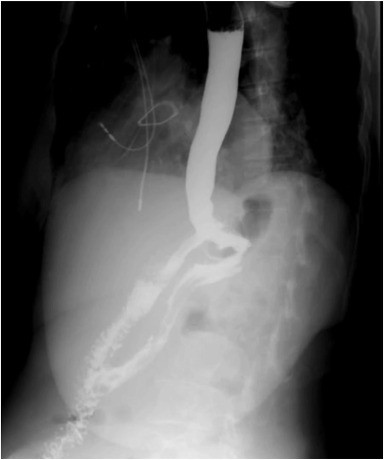
Upper GI series.
Read the full article online.
The information presented in Endoscopedia reflects the opinions of the authors and does not represent the position of the American Society for Gastrointestinal Endoscopy (ASGE). ASGE expressly disclaims any warranties or guarantees, expressed or implied, and is not liable for damages of any kind in connection with the material, information, or procedures set forth.
